EPISTAXIS …NASAL BLEEDING
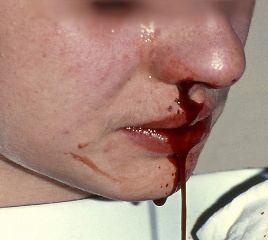
Epistaxis, or bleeding from the nose, is a common complaint. It is rarely life threatening but may cause significant concern, especially among parents of small children.[1] Most nosebleeds are benign, self-limiting, and spontaneous, but some can be recurrent. Many uncommon causes are also noted.
Epistaxis can be divided into 2 categories, anterior bleeds and posterior bleeds, on the basis of the site where the bleeding originates
Causes of epistaxis:
Causes of epistaxis can be divided into local causes (eg, trauma, mucosal irritation, septal abnormality, inflammatory diseases, tumors), systemic causes (eg, blood dyscrasias, arteriosclerosis, hereditary hemorrhagic telangiectasia), and idiopathic causes. Local trauma is the most common cause, followed by facial trauma, foreign bodies, nasal or sinus infections, and prolonged inhalation of dry air. Children usually present with epistaxis due to local irritation or recentupper respiratory infection (URI).
Trauma
Self-induced trauma from repeated nasal picking can cause anterior septal mucosal ulceration and bleeding. This scenario is frequently observed in young children. Nasal foreign bodies that cause local trauma (eg, nasogastric and nasotracheal tubes) can be responsible for rare cases of epistaxis.

Dry weather
Low humidity may lead to mucosal irritation. Epistaxis is more prevalent in dry climates and during cold weather due to the dehumidification of the nasal mucosa by home heating systems.
Drugs
Topical nasal drugs such as antihistamines and corticosteroids may cause mucosal irritation. Especially when applied directly to the nasal septum instead of the lateral walls, they may cause mild epistaxis. Medications such as nonsteroidal anti-inflammatory drugs (NSAIDs) are also frequently involved.
Septal abnormality
Septal deviations and spurs may disrupt the normal nasal airflow, leading to dryness and epistaxis.
Bacterial, viral, and allergic rhinosinusitis causes mucosal inflammation and may lead to epistaxis.
Tumors
Benign and malignant tumors can manifest as epistaxis.
Blood dyscrasias
Congenital coagulopathies should be suspected in individuals with a positive family history. Examples of congenital bleeding disorders include hemophilia and von Willebrand disease.
Acquired coagulopathies can be primary (due to the diseases) or secondary (due to their treatments). Among the more common acquired coagulopathies are thrombocytopenia and liver disease with its consequential reduction in coagulation factors. Even in the absence of liver disease, alcoholism has also been associated with coagulopathy and epistaxis. Oral anticoagulants predispose to epistaxis.
Vascular abnormalities
Arteriosclerotic vascular disease is considered a reason for the higher prevalence of epistaxis in elderly individuals.
Hereditary hemorrhagic telangiectasia
Vascular neoplasms, aneurysms, and endometriosis.
Migraine
Children with migraine headaches have a higher incidence of recurrent epistaxis than children without the disease.The Kiesselbach plexus, which is part of the trigeminovascular system, has been implicated in the pathogenesis of migraine.
Hypertension
The relationship between hypertension and epistaxis is often misunderstood. Patients with epistaxis commonly present with an elevated blood pressure. Epistaxis is more common in hypertensive patients, perhaps owing to vascular fragility from long-standing disease.
Hypertension, however, is rarely a direct cause of epistaxis. More commonly, epistaxis and the associated anxiety cause an acute elevation of blood pressure. Therapy, therefore, should be focused on controlling hemorrhage and reducing anxiety as primary means of blood pressure reduction.
Excessive coughing causing nasal venous hypertension may be observed in pertussis or cystic fibrosis.
Idiopathic causes
The cause of epistaxis is not always readily identifiable. Approximately 10% of patients with epistaxis have no identifiable causes even after a thorough evaluation.
The following precautions should be imparted to the patient:
· Use nasal saline spray.
· Avoid hard nose blowing or sneezing.
· Sneeze with the mouth open.
· Do not use nasal digital manipulation.
· Avoid hot and spicy foods.
· Avoid taking hot showers.
· Avoid aspirin and other NSAIDs.
The following simple instructions for self-treatment for minor epistaxis should be provided:
· Apply firm digital pressure for 5-10 minutes.

· Use an ice pack.
· Practice deep, relaxed breathing.
· Use a topical vasoconstrictor.