
AUTOIMMUNE DISEASES & THE NEED TO THE CONSULTANT
Autoimmune diseases & the need to the consultant
By Dr. Nashwa Elshaarawi
Consultant of Rheumatology
United Doctors Hospital
Many people think that the rheumatology clinics at hospitals take care only of one disease, which is the rheumatoid arthritis and that All will need treatment with cortisone therapy and end up at this point, but in deed the autoimmune connective tissue diseases (CTDS) represent a number of related conditions that include rheumatoid arthritis (RA), systemic lupus erythematosus(SLE) and the antiphospholipid (Hughes) syndrome, myositis, scleroderma, and Sjögren’s syndrome.
The main idea of the immune system is to fight the foreign invaders as viruses, bacteria; while in autoimmune disease the immune system starts auto-antibody production and starts to attack the body`s healthy tissue. These disorders are characterized by production of auto antibody and other immune-mediated dysfunction, with the presence of common clinical and serological features within some patients having multiple overlapping connective tissue disorders. Each of these diseases has a variety of auto-antibodies with its own classic presentation. The classic presentation of the disease can evolve slowly or rapidly to give the full picture of the disease to be diagnosed. Early in the disease presentation, whenever the full-blown picture of the disease is not yet definable, the disease at that time is diagnosed as undifferentiated CTD. While when more than one autoimmune CTD features presented in the same person; the condition is referred to overlap syndrome
In this article , I will discuss briefly one of the most common and most important disabilities which is the rheumatoid arthritis to be further continued later on to discuss the remaining disabilities in next following articles.
Rheumatoid arthritis (RA)
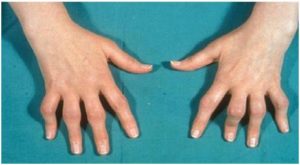
Rheumatoid arthritis (RA)is a chronic, disabling disease with considerable impact on patients’ lives. The world prevalence of RA might be around 0.3-1.2%. RA is characterized by persistent articular inflammation and proliferation of the synovial tissue, causing pain, stiffness, limitation of joint motion; although RA is associated with fatigue, anemia and sometimes fever. If untreated, most patients experience a chronic, fluctuating disease course that, despite therapy, may result in progressive deformity, disability, and premature death. The current management of RA involves early diagnosis and rapid, aggressive control of inflammation, aiming to prevent long-term joint destruction. This involves early use of disease-modifying antirheumatic drugs (DMARDs)and combination strategies, if no response switching to biological therapy according to the patient disease activity, and risk factors.
RA should be diagnosed as early as possible, mostly within the 1st 6 months from the onset of symptoms s the radio-graphic erosions tend to occur within the 1st year, hence treatment should start as soon as possible to halt the disease.




